Scoping review finds mixed evidence on suicide rates among dentists
Current evidence contradicts the assumption that dentistry has the highest suicide rate; but occupational stress and access to means remain real concerns for your workforce.
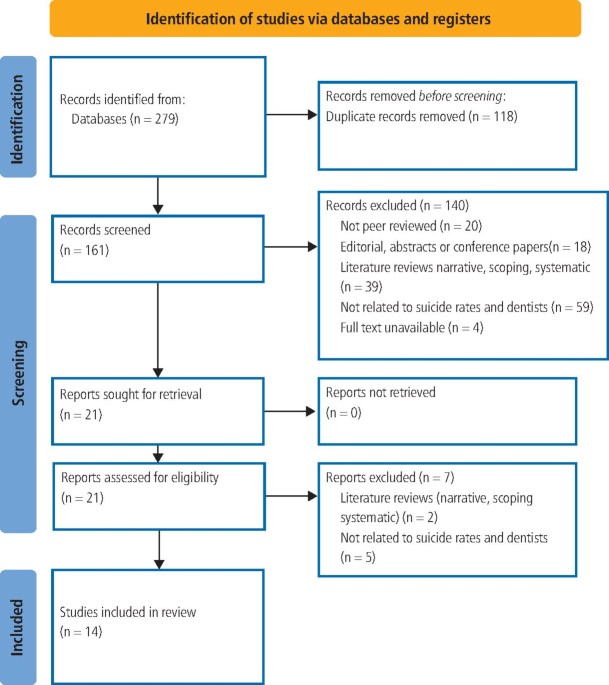
Evidence on dentist suicide rates remains inconsistent
A scoping review of 14 studies on suicide and suicidal ideation in the dental profession found conflicting evidence on whether dentists face elevated suicide risk compared to the general population. Three studies reported higher rates among dentists, while two found no difference or declining trends. Research spanned from 1960 to 2024 across Australia, Austria, Denmark, Norway, South Africa, Sweden, the USA and the UK. The heterogeneity reflects differences in study design, data sources, and changing attitudes toward mental health support over time.
Occupational stress, access to lethal means, and stigma drive risk
Across studies, occupational stress emerged as the dominant risk factor, including high workload, financial pressure, professional isolation, and perfectionism. Dentists' ready access to potent sedation and anaesthesia agents increases suicide attempt lethality. Mental health stigma within the dental profession remains a major barrier: fear of professional repercussions, licensure issues, and reputational damage deter practitioners from seeking care. Male dentists traditionally showed higher rates, but recent evidence indicates rising risk among women. Younger dentists facing early-career stress and older dentists experiencing late-career burnout appear particularly vulnerable.
Declining trends in some regions suggest interventions work
England saw a 59% reduction in dentist suicide mortality from 1979 to 2005, and Swedish rates peaked in the 1970s before declining by the 1980s. These trends coincide with enhanced mental health support, prevention initiatives, and improved working conditions. The review authors emphasize that reducing suicide risk requires profession-wide action: embedding mental health training in dental education, uncoupling help-seeking from punitive licensing consequences, strengthening controlled-substance protocols in practices, implementing peer support networks, and providing confidential access to care without career repercussions.
Frequently asked questions
Do dentists really have higher suicide rates than the general population?
Evidence is mixed. Three studies found elevated rates among dentists, while two found no difference or lower rates. Temporal trends in England and Sweden show declining rates in recent decades, suggesting improved support and workplace conditions have helped.
What are the main risk factors for suicide in dentistry?
The review identified occupational stress, access to lethal medications and tools, mental health stigma, professional isolation, financial pressure, and perfectionism as key factors. Male dentists historically showed higher rates; recent evidence indicates rising risk among women.
Why don't dentists seek help for mental health problems?
Fear of professional repercussions, licencing consequences, and reputational damage deter help-seeking. Stigma within the dental profession and concerns about confidentiality prevent many practitioners from disclosing distress or accessing care.
Which age groups of dentists face the highest suicide risk?
Younger dentists under 44 years old and those over 65 years old show elevated risk. Early-career stressors include educational debt and practice establishment; late-career factors include physical decline and identity changes approaching retirement.
What interventions have reduced suicide rates among dentists?
England and Sweden saw significant declines tied to enhanced mental health support, prevention initiatives, improved working conditions, confidential care pathways, peer support networks, and clear workplace policies separating treatment-seeking from impairment.