AI in aligner therapy: efficiency requires clinical oversight
Essential reading for clinicians using AI-assisted aligner planning. Explains why digital simulations fail and how to maintain clinical control.
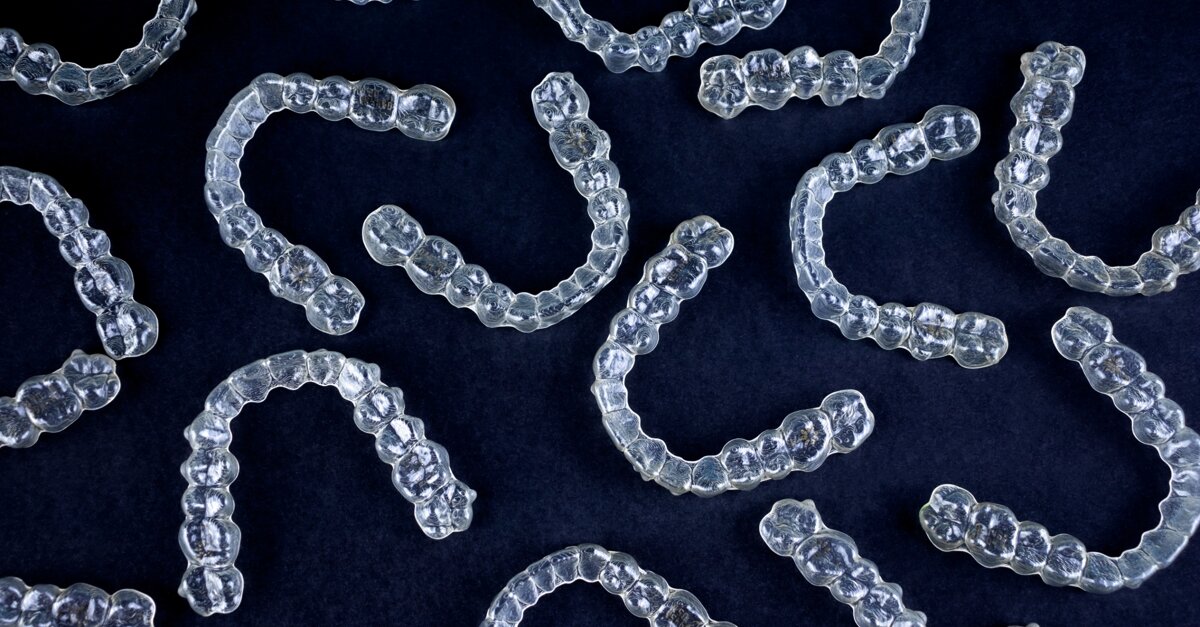
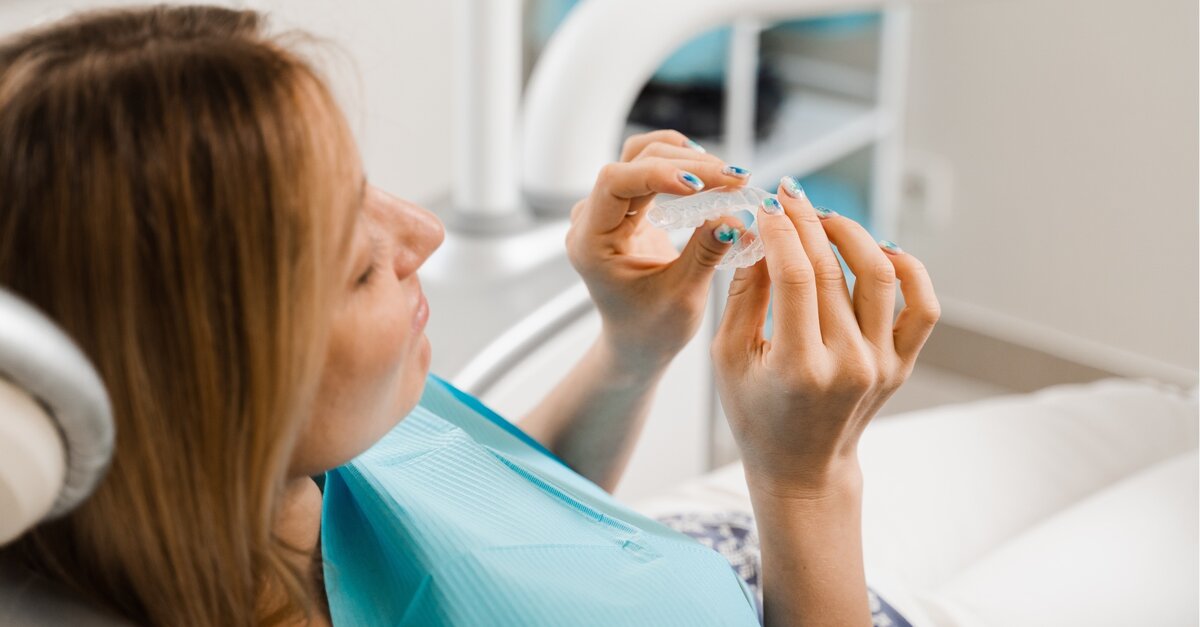
Artificial intelligence now assists with tooth segmentation, treatment planning, attachment placement and outcome prediction in aligner orthodontics. While AI-driven systems have dramatically improved workflow efficiency, generating treatment simulations in minutes, a growing gap exists between perfect digital animations and actual clinical results. Many clinicians experience treatment failures around the tenth to fifteenth aligner despite flawless digital set-ups, prompting the question: why does the simulation not match the outcome?
Where AI excels and where it falls short
AI performs exceptionally well on objective, binary classification tasks. Caries detection on radiographs exemplifies this strength: the question is clear, the criteria are measurable, and AI often matches or exceeds human performance. Orthodontic treatment planning, however, is fundamentally different. A single case typically admits multiple valid treatment strategies. Should the clinician expand the arch or perform interproximal reduction? Should incisor alignment prioritise aesthetics or occlusal stability? These trade-offs require clinical judgment and philosophy. AI systems identify statistically optimised patterns within historical datasets, but statistical optimisation is not clinical decision-making. The datasets themselves contain significant variation, trained on cases from thousands of clinicians with different experience levels, philosophies and finishing standards. AI cannot evaluate these differences the way clinicians do.
Digital models and biological reality
Digital treatment planning begins with intra-oral scans that must be segmented into individual teeth. This process involves estimation and interpolation where scan data is incomplete or ambiguous. While the resulting digital model appears mathematically precise, it remains an approximation of biology. Tooth segmentation errors influence predicted movement patterns. Additional abstraction layers follow: movements are staged digitally, attachments suggested automatically, collisions calculated computationally. Each step contributes to the final animation. Yet teeth move because forces are applied within biological limits, not because an animation shows movement. Biomechanics is often under-estimated in digital planning. Individual teeth may appear to move independently in simulations, but every force produces reactive forces elsewhere. Anchorage loss, vertical control issues and tracking failures often emerge during treatment, reflecting biological and mechanical complexity rather than software failure.
Maintaining clinical oversight in digital workflows
AI should support clinical decision-making, not replace it. Before reviewing a digital treatment set-up, the clinician must have clear diagnostic understanding and defined treatment objectives. Without this framework, the software may begin to guide the plan rather than serve it. Digital set-ups should be interpreted as proposals, not final plans. Clinicians must evaluate whether suggested movements are biomechanically realistic, whether anchorage requirements have been considered and whether the outcome aligns with treatment objectives. Efficiency combined with clinical oversight leads to more predictable outcomes. Efficiency without clinician-led decision-making risks turning treatment planning into automation.
Frequently asked questions
Why do perfect digital aligner simulations fail clinically?
Digital models are approximations of biological reality with inherent errors in tooth segmentation, interpolation and surface smoothing. Biomechanical complexity, anchorage requirements and reactive forces are often under-estimated in simulations. AI-generated plans reflect statistical patterns in training data, which may contain variation in clinical quality and philosophy.
What tasks does AI perform best in orthodontic dentistry?
AI excels at objective, binary classification tasks with defined parameters, such as caries detection on radiographs. It can identify occlusal deviations and anatomical norms. However, it performs poorly at treatment planning, which requires clinical judgment and involves multiple valid strategies with trade-offs.
How should clinicians interpret AI-generated aligner treatment set-ups?
Treat digital set-ups as proposals, not final plans. Evaluate whether suggested movements are biomechanically realistic, whether anchorage has been considered and whether the outcome aligns with your treatment objectives. Maintain critical perspective before and after reviewing the software recommendation.
What role should AI play in aligner orthodontics?
AI should support clinical decision-making, not replace it. It enhances workflow efficiency, aids diagnostics and streamlines digital planning. The clinician remains responsible for diagnosis, judgment, treatment philosophy and patient outcomes. Combining efficiency with clinical oversight produces the most predictable results.
Why do aligner systems fail around the tenth to fifteenth aligner?
Tracking failures, anchorage loss and vertical control issues typically emerge when biomechanical complexity exceeds what the digital simulation accounted for. Reactive forces, interdependencies between teeth and biological limits on movement are often underestimated in AI-generated plans.