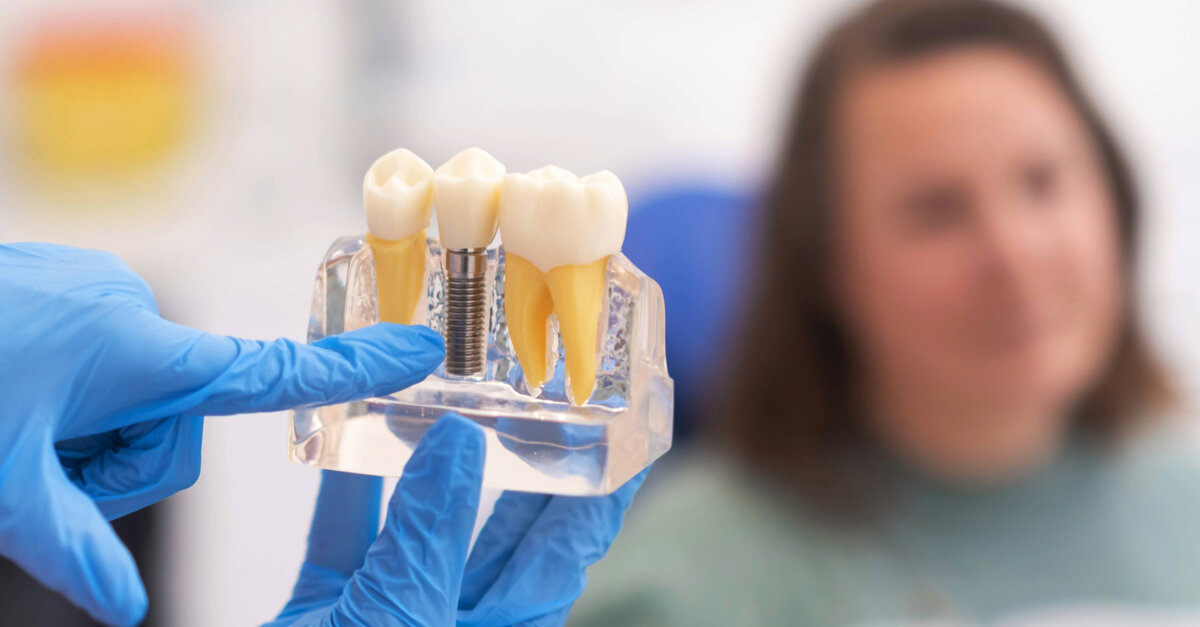
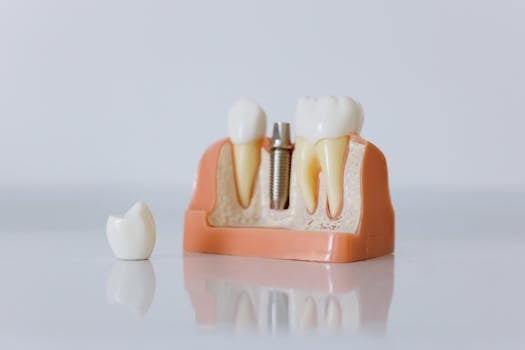
Digital scan errors stem from geometry control, not scanner quality
Reference geometry controls scan accuracy more than device choice; protocol structure prevents costly remakes in all-on-X cases.
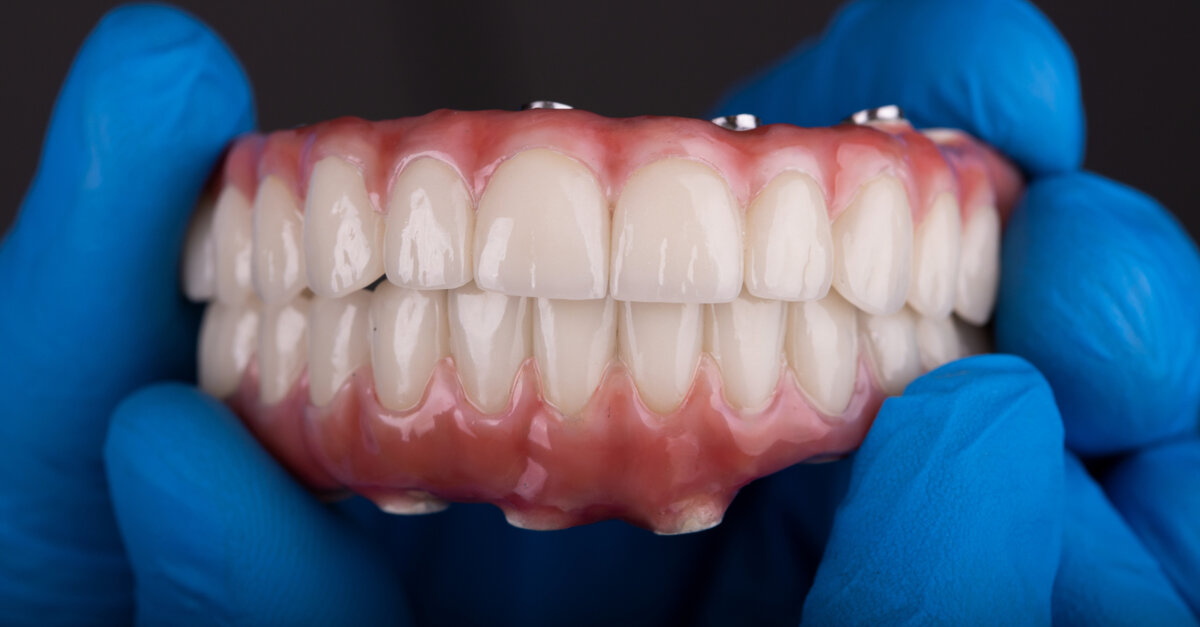
Prof. Adam Nulty, a leading expert in digital implant workflows, argues that scanning errors in all-on-X dentistry are driven by poor geometry control rather than technology limitations. Speaking ahead of his IDEM 2026 lecture in Singapore, Nulty highlights that clinicians often overlook critical spatial relationship capture in favour of assuming scanner resolution determines accuracy.
Where digital workflows lose accuracy
Accuracy failures occur most frequently during intra-oral scan acquisition in edentulous arches and during dataset merging, when combining intra-oral scans with CBCT, facial scans, or prosthetic design data. Intra-oral scanners rely on optical stitching, which becomes unreliable over large, feature-poor areas such as edentulous ridges. When multiple datasets are merged, each may be individually accurate, but best-fit approximation during merging introduces cumulative spatial error. The core problem is not scanner brand or resolution but how small inaccuracies propagate across datasets.
Reference-based scanning maintains alignment
Structured protocols such as Scan Ladder address these errors by prioritising geometric alignment over surface stitching. The workflow begins with rigid, irregular geometric landmarks captured before soft tissue, allowing the scanner to build datasets from a known spatial framework rather than approximation. This controls drift at source and provides consistent reference systems across datasets, improving merging reliability. Nulty emphasises that well-executed reference-based workflows are statistically comparable to photogrammetry but without associated hardware costs or workflow burden.
Streamlining accuracy without added complexity
Clinicians may worry that introducing reference geometry increases chair time, but structured workflows typically reduce remakes, verification jigs, and additional appointments. Starting with geometry adds seconds rather than minutes but avoids hours of downstream correction. Industry developments include real-time geometric recognition, improved cross-dataset registration tools such as fiducial markers, and greater emphasis on reference geometry. Nulty calls for wider adoption of standardised geometric reference systems, better education on scanning protocols across entire workflows, and less fragmentation between hardware, software, and prosthetic libraries.
Frequently asked questions
Why do intra-oral scans fail in edentulous arch cases?
Intra-oral scanners rely on optical stitching, which becomes unreliable over large, feature-poor areas like edentulous ridges. Common errors include scanning soft tissue first, introducing drift at the start, and failing to establish stable reference geometry early in the sequence.
How do small scanning errors accumulate in full-arch cases?
Small errors are not isolated in full-arch scanning. When multiple datasets are merged (intra-oral scan with CBCT, facial scan, or prosthetic data), each may be individually accurate, but best-fit approximation during merging introduces cumulative spatial error across the entire arch.
What is the Scan Ladder workflow and how does it improve accuracy?
Scan Ladder is a reference-based protocol that begins by capturing rigid, irregular geometric landmarks before soft tissue, building the dataset from a known spatial framework rather than approximation. This controls drift at source and provides consistent reference systems across datasets, improving merging reliability and comparing to photogrammetry outcomes.
Does adding reference geometry to scanning increase chair time?
No. Starting with geometry typically adds only seconds but avoids hours of downstream correction, remakes, and additional appointments. Structured, geometry-led workflows reduce re-scans, improve first-time fit, and simplify laboratory communication.
What development would most improve dataset alignment in digital workflows?
Prof. Nulty advocates for wider adoption of standardised geometric reference systems, better education on scanning protocols across entire workflows, and less fragmentation between hardware, software, and prosthetic libraries to ensure the digital position of implants matches reality.