King's College study finds over one-third of dental patients have undiagnosed diabetes risk
King's College study shows dental appointments can screen for undiagnosed diabetes; practical implications for patient referral pathways.
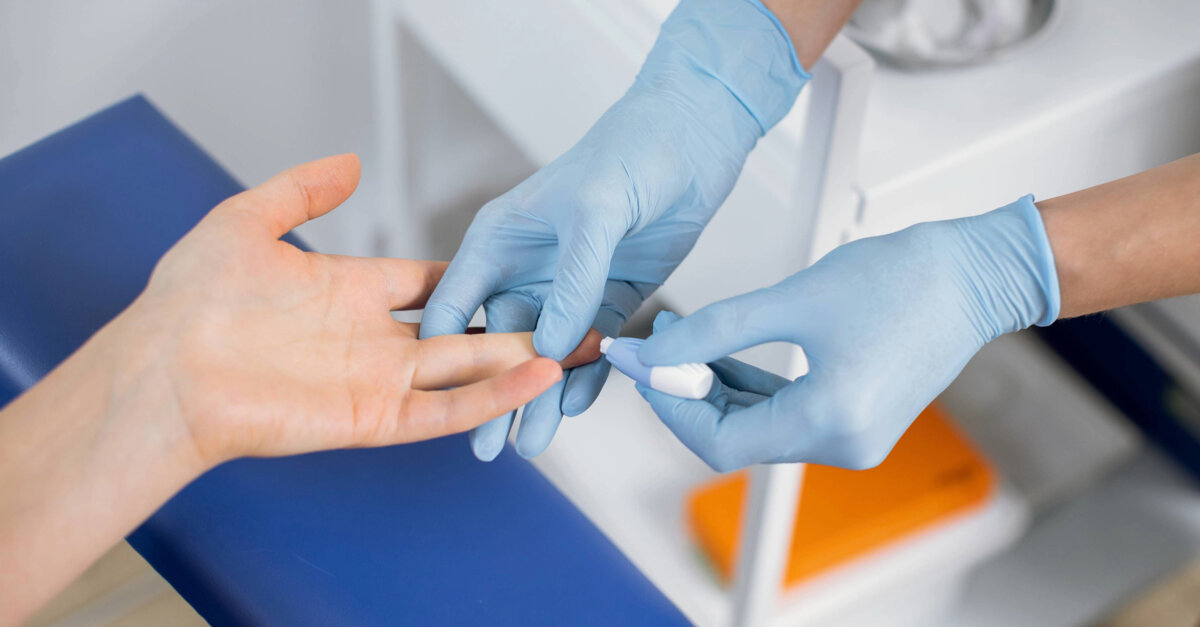
Chairside screening identifies undiagnosed metabolic disease in dental settings
A study from King's College London examined the use of rapid haemoglobin A1c (HbA1c) testing during routine dental appointments. Researchers tested over 900 patients in a secondary care dental setting and found that more than one-third showed blood glucose levels consistent with prediabetes or diabetes. The finger prick HbA1c test measures average blood glucose over two to three months and delivers results within minutes without requiring fasting, making it practical for use during standard appointments.
Implications for early detection and patient referral
Dental services reach patients who may not routinely attend primary care, offering an alternative pathway for identifying chronic disease early. When elevated HbA1c levels are detected, patients can be referred to their general medical practitioner for confirmatory diagnosis and management. Lead author Dr Mark Ide noted that most patients in the study were surprised to learn they had elevated HbA1c levels and were unaware of their prediabetes or diabetes risk. The findings suggest dental teams can contribute more actively to early identification of metabolic disease and support integrated, preventive care.
Periodontal disease and screening considerations
The study examined whether periodontal status might help identify which patients are most appropriate for diabetes screening. Researchers found that elevated HbA1c levels were associated with increasing severity of periodontal disease, but this relationship weakened when other factors were taken into account. This suggests that periodontal severity alone may have limited value as an independent trigger for testing. The authors noted their findings are based on a specific patient group with high prevalence of periodontitis, which may limit generalisation to other dental populations. A separate UK study called INDICATE-2 is now evaluating a dental care pathway in 50 high-street practices involving diabetes risk assessment and referral where appropriate.
Frequently asked questions
Can dental teams screen for undiagnosed diabetes during appointments?
Yes, according to King's College London research. Rapid finger prick HbA1c testing can be performed chairside during routine appointments without fasting. Results are available within minutes, making it practical for identifying patients with elevated blood glucose levels consistent with prediabetes or diabetes.
What percentage of dental patients in the study had undiagnosed prediabetes or diabetes?
More than one-third of dental patients with no prior diabetes diagnosis showed blood glucose levels consistent with prediabetes or diabetes when tested during routine appointments in the King's College study of over 900 patients.
Is periodontal disease severity a reliable indicator for diabetes screening?
The King's study found that while elevated HbA1c levels were associated with increasing periodontal disease severity, this relationship weakened when other factors were considered. Periodontal severity alone may have limited value as an independent trigger for diabetes testing.
What should happen after a chairside diabetes screening reveals elevated HbA1c?
Patients with elevated HbA1c levels detected in dental settings should be referred to their general medical practitioner for confirmatory diagnosis and management. The study notes that many patients were unaware of their diabetes or prediabetes risk before the dental screening.
How does the INDICATE-2 study relate to dental diabetes screening?
The University of Birmingham's INDICATE-2 study is evaluating a dental care pathway in 50 UK high-street practices that includes diabetes risk assessment and finger prick HbA1c testing, with referral to medical care where appropriate.